As healthcare systems continue to evolve, people are increasingly seeking solutions that are not only connected and accessible, but also intelligent enough to support faster, safer, and more personalized care.
At the same time, healthcare is rapidly shifting from reactive treatment toward proactive prevention and smarter care delivery. This is where AI-powered devices are becoming the driving force behind this transformation.
One example of this shift can be seen through solutions like the SmartFuture MediKit, an AI-powered health monitoring system designed to support home care, remote patient monitoring, and more connected healthcare experiences.
Rather than relying solely on occasional clinic visits or waiting until symptoms become more serious, many individuals, families, and healthcare providers are beginning to explore smarter ways to stay informed, prepared, and more proactive in managing daily health. Here’s why this approach is gaining attention.
1. Prevent Health Issues Before They Escalate
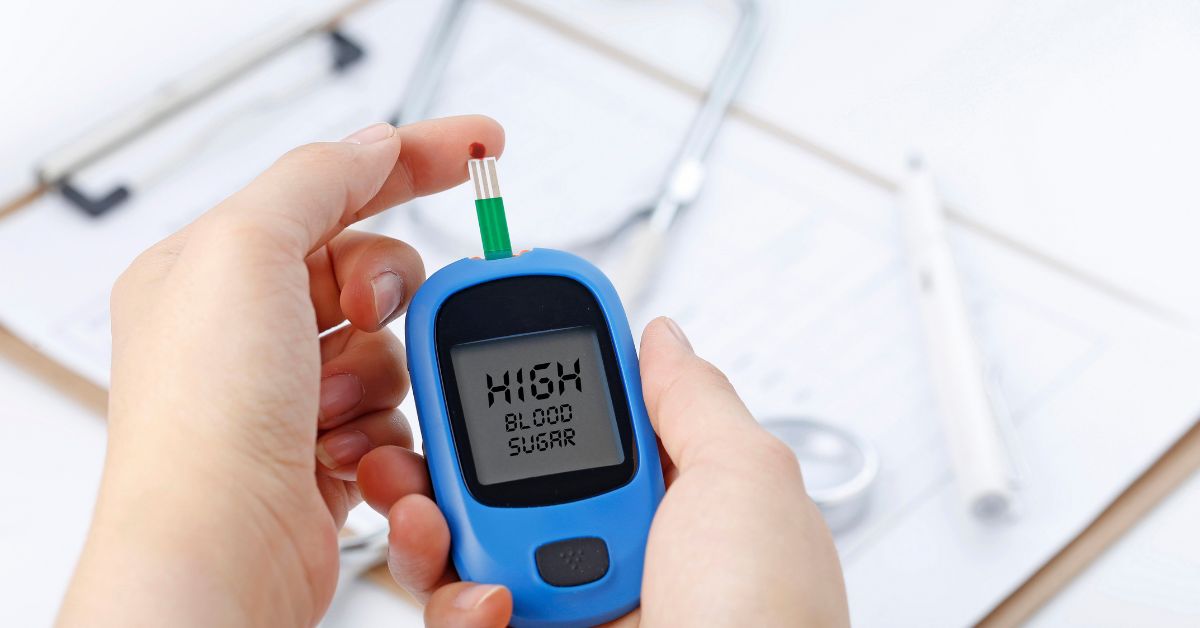
Serious conditions such as hypertension, cardiovascular disease, and respiratory complications often develop silently over time. Unfortunately, without consistent monitoring, these early warning signs can easily go unnoticed until they become more critical.
This is where SmartFuture MediKit plays an important role. By enabling continuous daily tracking of vital health data, the platform helps users detect irregularities earlier and respond more proactively.
Rather than simply collecting readings, the system uses AI-powered analytics and predictive machine learning (ML) to identify patterns, trends, and potential health risks before they escalate further. As a result, users now can have data-driven care at home or anywhere.
Ultimately, early awareness leads to earlier action and in many cases, better long-term outcomes.
2. All-in-One AI-Powered Smart Health Monitoring Device
Managing multiple standalone medical devices can often feel inconvenient, fragmented, and difficult to maintain consistently. To solve this challenge, SmartFuture MediKit combines essential health monitoring tools into one connected ecosystem, including:
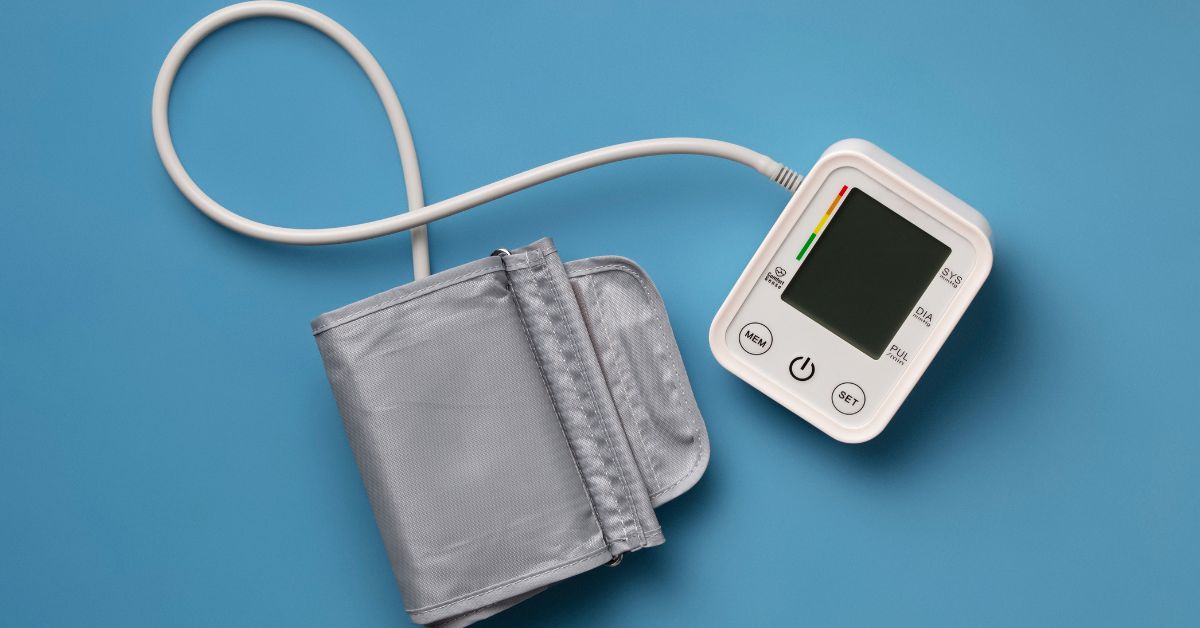
- Blood pressure monitor
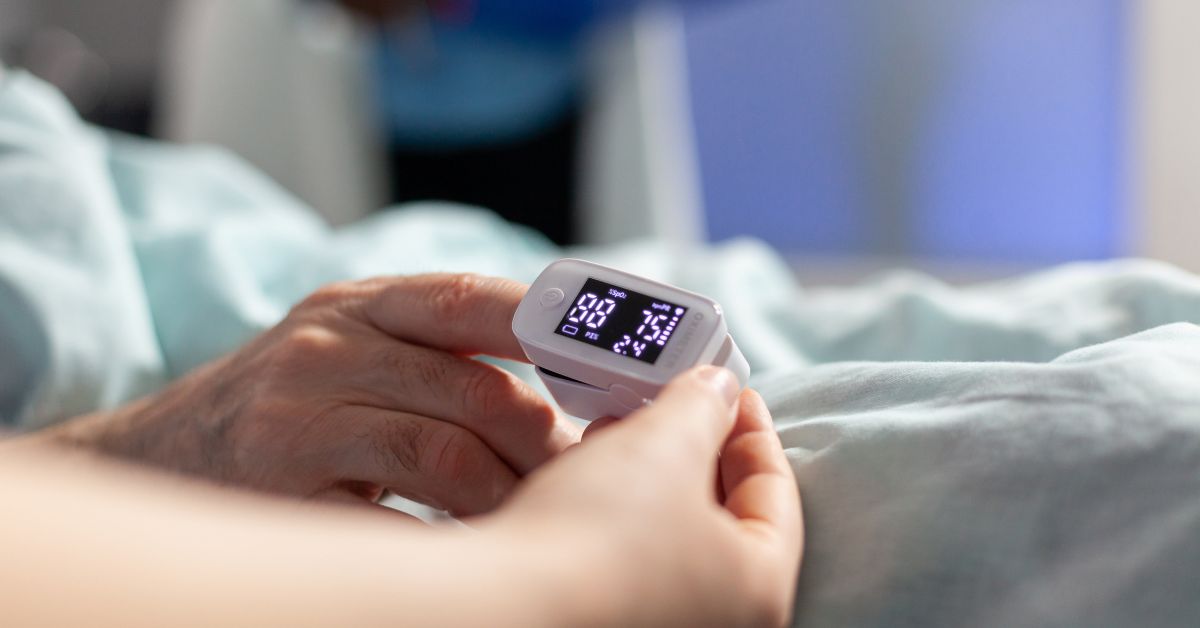
- Pulse oximeter (oxygen saturation monitor)
- Thermometer
- Portable ECG device
However, the value of MediKit goes beyond hardware integration alone. Powered by AI technologies such as Computer Vision and OCR (Optical Character Recognition), the platform can intelligently digitize and interpret medical records, prescriptions, health reports, and device readings. This helps reduce manual data entry while simultaneously improving operational efficiency and healthcare accuracy.
In addition, all collected health information is centralized into one platform, making it easier for users, caregivers, and healthcare professionals to access a clearer and more comprehensive view of overall health conditions in real time.
3. Real-Time Monitoring with AI-Driven Health Insights
Traditional healthcare systems typically rely on periodic checkups. However, health conditions can change at any moment. Not only during scheduled appointments.
SmartFuture MediKit addresses this gap through continuous real-time health monitoring, enabling users and caregivers to monitor vital signs more consistently and effectively from anywhere.
More importantly, the platform is enhanced with Clinical AI capabilities that help transform raw health data into meaningful and actionable insights. Instead of viewing isolated numbers, users and healthcare providers can better understand health fluctuations, emerging abnormalities, and potential risks.
At the same time, predictive machine learning continuously learns from ongoing health data, helping identify unusual patterns that may require earlier medical attention.
In critical situations, these real-time AI-supported insights can contribute to faster decision-making, quicker intervention, and improved patient outcomes.
4. Designed for Simplicity, Accessibility, and Everyday Use
One of the biggest challenges with healthcare technology is usability. Many monitoring devices fail to deliver long-term value because they are overly complex, difficult to set up, or confusing for everyday users.
To overcome this, SmartFuture MediKit is intentionally designed with simplicity and accessibility in mind. Key features include:
- Simple and user-friendly interface
- Fast and minimal device setup
- Clear and easy-to-read health dashboards
- AI-assisted guidance for better health understanding
In addition, the platform incorporates Natural Language Processing (NLP) technology to help simplify medical communication. Complex healthcare information and technical data can be translated into more understandable insights, making health monitoring easier for users, caregivers, and even elderly individuals who may not have medical backgrounds.
As a result, MediKit becomes more practical for daily use across different lifestyles and age groups. This including families, senior citizens, athletes, and busy professionals managing health from home.
And because the system is easier to use consistently, it also helps encourage better long-term health awareness and engagement.
5. Enables Remote Patient Monitoring and Connected Care
Today, healthcare is no longer limited to hospitals and clinics alone. With the continued growth of telehealth and digital healthcare ecosystems, remote patient monitoring has become increasingly essential.
SmartFuture MediKit supports this transformation by enabling:
- Continuous monitoring of vital health data
- Secure sharing of information with healthcare providers
- AI-supported health trend analysis
- Ongoing care beyond traditional clinical environments
By integrating Clinical AI, predictive analytics, and connected monitoring systems, the platform helps bridge the gap between patients, caregivers, and healthcare professionals regardless of location.
Consequently, patients can remain connected, monitored, and supported more consistently, while healthcare providers gain better visibility into patient conditions between visits.
This creates a more connected, efficient, and proactive healthcare experience overall.
The Future of Healthcare Starts at Home
The growing adoption of the SmartFuture MediKit reflects a larger shift in how people approach healthcare today. Increasingly, individuals are seeking more control, greater visibility, and smarter tools to support their daily health decisions.
By combining preventive monitoring, AI-powered technologies, real-time health insights, and connected care systems, SmartFuture MediKit empowers users to stay one step ahead of potential health risks.
From Computer Vision and OCR to Clinical AI, Predictive Machine Learning, and Natural Language Processing, the platform represents how intelligent healthcare solutions are reshaping the future of care delivery.
Healthcare is no longer only about treatment. It is increasingly about prevention, consistency, accessibility, and smarter living powered by AI.
Get Started with SmartFuture MediKit

Take control of your health, before it becomes urgent.
We’d love to support your journey:
📧 sales@oursmartfuture.com
📧 developer@oursmartfuture.com
📞 +65 8836 0984 (Mon–Fri, 10 AM–6 PM)
💬 Chat with us on WhatsApp for a quicker reply
Or visit us at:
📍 246 Macpherson Road, #03-01 Betime Building, Singapore 348578
📍 651 N Broad St, Suite 201, Middletown, Delaware 19709
























 +65 8836 0984
+65 8836 0984 sales@oursmartfuture.com
sales@oursmartfuture.com 246 Macpherson Road, #03-01 Betime
246 Macpherson Road, #03-01 Betime 




