AI in healthcare is becoming increasingly important as healthcare providers around the world continue to face growing and complex challenges.
On one hand, patient demand is rising rapidly. Meanwhile, healthcare professionals are also experiencing increasing levels of burnout, operational pressure, and growing expectations to deliver faster, more personalized, and more efficient care.
Recent regulatory developments, in countries like Singapore, where updated healthcare AI governance guidelines were introduced to support responsible AI adoption. It reflects a broader global movement toward safer, more transparent, and more structured AI implementation in healthcare environments.
Because of this momentum, healthcare organisations are now showing stronger interest in AI-powered solutions for:
- Patient monitoring
- Clinical triage
- Risk scoring
- Rehabilitation support
- Workflow automation
More importantly, this shift signals an important industry reality: healthcare can no longer rely solely on reactive care models. Instead, providers are moving toward proactive, data-driven, and preventive approaches to patient care.
Why Healthcare Providers Are Turning to AI
Traditionally, healthcare systems have depended heavily on manual reviews, delayed symptom reporting, and clinician-intensive processes. As a result, healthcare teams often spend significant amounts of time reviewing repetitive data, prioritizing cases manually, and responding only after conditions worsen.
However, patient volumes continue increasing while healthcare resources remain limited. In addition, clinicians are now expected to review larger amounts of patient data, monitor more remote cases, and respond faster to deteriorating conditions across multiple care settings.
This is where AI becomes increasingly valuable.
Rather than replacing healthcare professionals, modern healthcare AI acts as a decision-support layer that helps improve visibility, speed up triaging, and identify risks earlier. In other words, AI helps healthcare teams prioritize attention where it matters most.
At the same time, healthcare organizations are also becoming more focused on implementing AI responsibly. As AI adoption accelerates, there is growing emphasis on:
- Human oversight
- Patient safety
- Transparent decision-making
- Clinically accountable AI systems
Therefore, the goal of healthcare AI is not automation for the sake of replacing people, but rather enabling clinicians to work more efficiently while improving patient outcomes.
How SmartFuture Integrates AI in Healthcare Solutions
As demand for intelligent healthcare systems grows, SmartFuture has been actively developing AI-powered healthcare devices and digital health solutions designed to support modern clinical workflows and remote patient care.
SmartFuture’s ecosystem combines:
- AI-powered Remote Patient Monitoring (RPM)
- Intelligent patient scoring systems
- Predictive health monitoring
- Conversational rehabilitation support
- AI-assisted triaging
- Smart healthcare dashboards
- Automated health data collection
Through connected devices and intelligent healthcare software, SmartFuture enables healthcare providers to monitor patient conditions more proactively and efficiently.
Instead of relying solely on periodic check-ups, SmartFuture’s AI-powered solutions allow healthcare teams to receive continuous patient insights through real-time data collection and predictive analysis.
This creates a more connected, responsive, and preventive healthcare experience for both clinicians and patients.
AI-Powered Patient Monitoring Enables Earlier Intervention

One of the fastest-growing applications of healthcare AI is predictive patient monitoring and this is one of the key areas where SmartFuture’s AI-powered ecosystem plays an important role.
SmartFuture devices and monitoring platforms can continuously analyze multiple health indicators simultaneously, including:
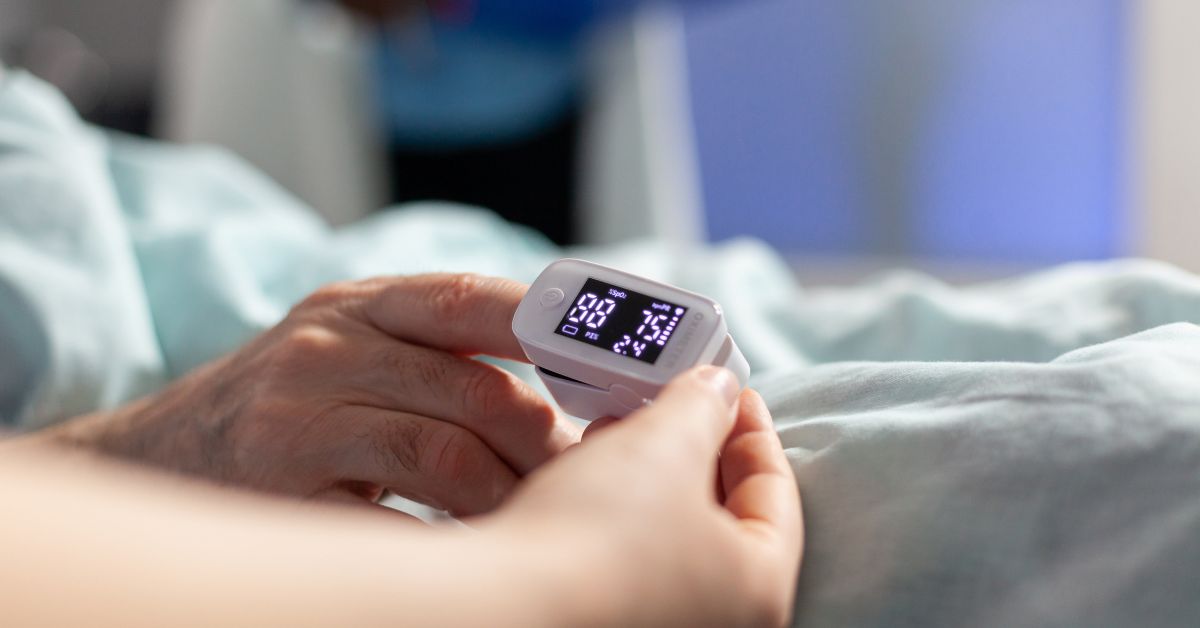
- Oxygen saturation (SpO₂)
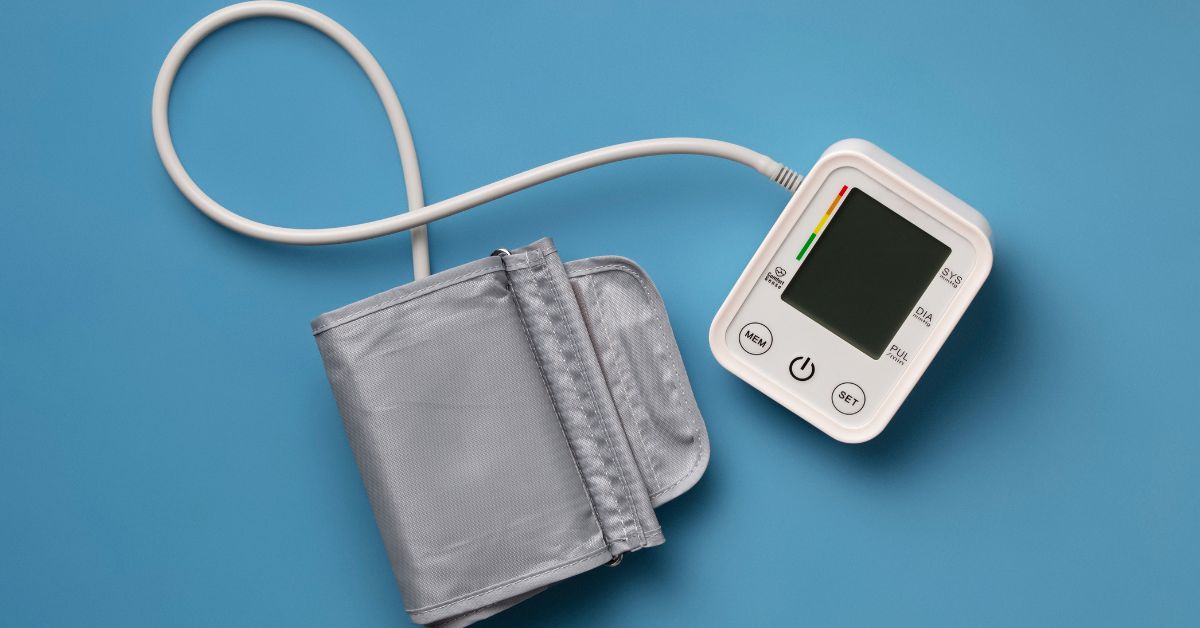
- Blood pressure
- Heart rate trends
- Rehabilitation adherence
- Patient questionnaires
- Symptom progression
By analysing these signals together, machine learning models can detect early deterioration patterns before conditions become critical.
For example, if a rehabilitation patient begins reporting worsening breathlessness while oxygen levels gradually decline, SmartFuture’s AI monitoring system can automatically prioritize that patient for clinical review before the situation escalates further.
As a result, healthcare teams can:
- Detect deterioration earlier
- Reduce avoidable hospital readmissions
- Prioritize high-risk patients faster
- Improve care response times
- Reduce monitoring blind spots
For patients, this creates a far more proactive healthcare experience. Instead of waiting until symptoms become severe, patients can receive earlier attention, intervention, and ongoing support.
AI in Healthcare Clinical Triage Helps Minimize Delays and Improve Care Efficiency

In addition to patient monitoring, AI-assisted clinical triage is another area where SmartFuture solutions help improve healthcare efficiency.
Traditionally, clinicians manually review patient questionnaires, symptoms, and vital signs to determine urgency levels. However, this process becomes increasingly difficult at scale — especially in remote care programs, rehabilitation services, and chronic disease management.
To address this challenge, SmartFuture’s AI-assisted triage systems can automatically analyze patient submissions and generate intelligent risk scores based on:
- Symptom severity
- Vital sign abnormalities
- Historical trends
- Rehabilitation progression
- Risk escalation patterns
Because of this, care teams can focus their attention on patients who require intervention most urgently.
Rather than reviewing every patient equally, clinicians can instead prioritize:
- High-risk deterioration cases
- Patients with worsening symptoms
- Patients requiring immediate review
- Cases needing escalation before complications occur
Importantly, AI does not replace medical judgment. Final clinical decisions still remain with healthcare professionals.
Instead, SmartFuture’s AI solutions reduce administrative burden while enabling clinicians to work more efficiently with better visibility across patient populations.
Conversational AI Improves Rehabilitation Adherence

Beyond monitoring and triage, SmartFuture also integrates conversational AI into rehabilitation support workflows.
Many rehabilitation programs struggle with:
- Missed sessions
- Poor exercise consistency
- Low patient engagement
- Limited follow-up outside clinical settings
To help address this issue, SmartFuture’s AI-powered rehabilitation companion supports patients throughout their recovery journey by providing:
- Exercise reminders
- Symptom check-ins
- Educational reinforcement
- Rehabilitation guidance
- Frequently asked question support
As a result, patients experience a more continuous and connected care journey beyond hospital visits alone.
For patients recovering from cardiovascular, pulmonary, or orthopaedic conditions, stronger engagement often leads to better rehabilitation outcomes and more consistent recovery progress over time.
Healthcare AI Must Be Safe, Transparent, and Human-Centeredd
As AI adoption continues accelerating globally, healthcare organizations are also recognizing the importance of responsible implementation.
Ultimately, the most effective healthcare AI systems are not designed to replace clinicians. Instead, they are designed to:
- Support faster clinical decisions
- Improve patient monitoring
- Reduce operational burden
- Enable earlier intervention
- Enhance patient engagement
With AI-powered healthcare devices, predictive monitoring systems, intelligent dashboards, and rehabilitation support solutions, SmartFuture is helping healthcare providers modernize patient care while maintaining a human-centered approach.
Therefore, the conversation is no longer about whether AI belongs in healthcare.
Instead, the focus is now shifting toward how healthcare organisations can implement AI responsibly to improve patient outcomes, clinician efficiency, and long-term care sustainability.
Ready to Explore AI-Powered Healthcare Solutions?
As healthcare providers continue modernising patient care, AI-powered monitoring, triage, and rehabilitation systems are becoming increasingly essential for improving efficiency, patient engagement, and clinical outcomes.
If your organisation is exploring AI implementation for healthcare workflows, remote patient monitoring, or intelligent rehabilitation support, SmartFuture is ready to help. Contact us now!
📧 sales@oursmartfuture.com
📧 developer@oursmartfuture.com
📞 +65 8836 0984 (Mon–Fri, 10 AM–6 PM)
💬 Chat with us on WhatsApp for a faster response
Visit Us
📍 Singapore: 246 Macpherson Road, #03-01 Betime Building 348578
📍 USA: 651 N Broad St, Suite 201, Middletown, Delaware 19709



























 +65 8836 0984
+65 8836 0984 sales@oursmartfuture.com
sales@oursmartfuture.com 246 Macpherson Road, #03-01 Betime
246 Macpherson Road, #03-01 Betime 




